
Jacobs V, May HT, Bair TL, Crandall BG, Cutler MJ, Day JD, et al. Rates, management, and outcome of rivaroxaban bleeding in daily care: results from the Dresden NOAC registry. 2014 12(3):320–8.īeyer-Westendorf J, Förster K, Pannach S, Ebertz F, Gelbricht V, Thieme C, et al. Effectiveness and safety of novel oral anticoagulants as compared with vitamin K antagonists in the treatment of acute symptomatic venous thromboembolism: a systematic review and meta-analysis. Van der Hulle T, Kooiman J, den Exter PL, Dekkers OM, Klok FA, Huisman MV. Comparison of the efficacy and safety of new oral anticoagulants with warfarin in patients with atrial fibrillation: a meta-analysis of randomised trials. Ruff CT, Giugliano RP, Braunwald E, Hoffman EB, Deenadayalu N, Ezekowitz MD, et al. Non-vitamin K antagonist oral anticoagulation agents in anticoagulant naïve atrial fibrillation patients: danish nationwide descriptive data 2011–2013. Olesen JB, Sørensen R, Hansen ML, Lamberts M, Weeke P, Mikkelsen AP, et al. Trends in utilization of warfarin and direct oral anticoagulants in older adult patients with atrial fibrillation. Pharmacology and management of the vitamin k antagonists*: American college of chest physicians evidence-based clinical practice guidelines (8th edition). 2015 13(Suppl 1):S266–71.Īnsell J, Hirsh J, Hylek E, Jacobson A, Crowther M, Palareti G. Warfarin pharmacogenomics: current best evidence. Acenocoumarol and heparin compared with acenocoumarol alone in the initial treatment of proximal-vein thrombosis. Underuse of oral anticoagulants in atrial fibrillation: a systematic review. Ogilvie IM, Newton N, Welner SA, Cowell W, Lip GYH. Guidance for the practical management of warfarin therapy in the treatment of venous thromboembolism. Witt DM, Clark NP, Kaatz S, Schnurr T, Ansell JE. Erratum to: pharmacology of anticoagulants used in the treatment of venous thromboembolism. Nutescu EA, Burnett A, Fanikos J, Spinler S, Wittkowsky A. 
Evidence-based management of anticoagulant therapy: antithrombotic therapy and prevention of thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines. Holbrook A, Schulman S, Witt DM, Vandvik PO, Fish J, Kovacs MJ, et al. Oral anticoagulant therapy: antithrombotic therapy and prevention of thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines. KeywordsĪgeno W, Gallus AS, Wittkowsky A, Crowther M, Hylek EM, Palareti G. In this chapter, we will discuss the pharmacology, clinical utility, and practical management aspects that promote optimized safety and efficacy of warfarin therapy. Thus, clinicians must possess familiarity with this still widely used medication. 
While direct oral anticoagulants (DOACs) have significantly changed approaches to anticoagulation therapy, are more convenient and are easier to use, warfarin will continue to be a mainstay of therapy for many patients. 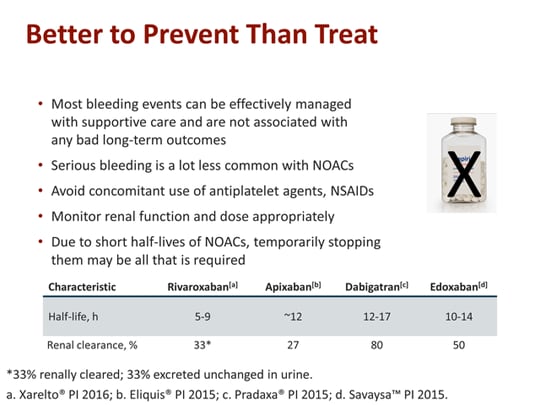
These drawbacks have historically resulted in under treatment of patients that warrant anticoagulation therapy (Ogilvie et al., Am J Med. 
Although very effective for prevention and treatment of venous and arterial thromboembolism, warfarin has a narrow therapeutic index, many drug, disease, and dietary interactions, and requires frequent monitoring and dose adjustments (Ageno et al., Chest 141(2 Suppl):e44S–88S, 2012 Holbrook et al., Chest 141(2 Suppl):e152S–84S, 2012 Nutescu et al., J Thromb Thrombolysis 42(2):296–311, 2016 Witt et al., J Thromb Thrombolysis 41:187–205, 2016). Until recently, vitamin K antagonists, such as warfarin, were the only oral anticoagulants available for long-term or extended anticoagulation. 
0 Comments
Leave a Reply. |



 RSS Feed
RSS Feed
